- Postgraduate Research Student
- Australian Venom Research Unit
- Department of Pharmacology, School of Medicine,
- University of Melbourne
Research Questions
This project examines the key question of how the burden from snakebite can be dealt
with most effectively and efficiently by developing nations, such as
Papua New Guinea.
In order to answer this question it is essential that a fundamental understanding of the state
of health infrastructure and administration, and its capacity to make
dynamic responses to health issues be sought out. To obtain this measure of
systems performance the research needs to explore not just the clinical
fundamentals of snakebite, but also the larger health service framework
within which the problem must be addressed.
In the case of Papua New Guinea a fractured and largely ineffectual health service is as much to
blame for high morbidity and mortality as are problems experienced in the
individual clinical management of each snakebite emergency. Resolving the
question of how to deal with the high human and financial costs of the
problem necessitates a broad approach encompassing epidemiological,
clinical, zoological, toxinological and public health management research.
The projects undertaken during this candidature for Doctor of Philosophy
seek to accumulate the answers to individual questions that will
cumulatively provide practical and sustainable solutions to the broader
issues that apply not just in Papua New Guinea, but in many other of the
world’s tropical developing nations.
Specifically this project will seek to resolve a number of questions:
-
How best can quantitative measures of injury burden, such as crude incidence and
mortality at regional, provincial and national levels be reliably
measured, and what systems can be established to facilitate surveillance
and dynamic monitoring within the health infrastructure?
-
Who are the culprits? Which species of venomous snakes are responsible for injury in
particular regions of the country? What relationships exist between
populations and are all populations homogenous, or do significant
variations in phylogeny translate to significant variations in venom
composition and clinical syndromes?
-
What are the clinical syndromes of envenomation at species level? How are these
conditions managed? What sustainable improvements to the clinical care
of patients and to the operations of service delivery systems can be
made that will produce tangible benefits in the form of reduced
morbidity and mortality at all levels of the system?
-
Can public education and first aid training be effective tools for reducing the
incidence of snakebite, and for improving the prognosis of the
snake-bitten? Can the techniques of snakebite first aid be successfully
taught to those in most need of these skills, and what is the efficacy
of the training approach?
-
Does ongoing professional training, education and access to information functionally
improve the skills of the medical and paramedical workforce? Can we
measure tangible improvements in the outcomes for envenomed patients
over time? Does a structured program of training combined with
standardisation of treatment protocols and procedures translate into
real improvement in patient prognosis?
-
Can we develop a model system in Papua New Guinea for the successful sustainable
management of resources such as antivenoms? Can the rising costs of
treatment be curtailed by a coordinated national approach and the
establishment of local research and clinical capacity? Can new avenues
for reducing cost and maintaining the supply of antivenoms be
established within nations such as Papua New Guinea, and can a
successful international model be established through cooperation with
more affluent neighbours or through strategic regional alliances?
Can all of these approaches, collectively, be maintained, and can lives be saved?
Summary and analysis of relevant literature
Note: A comprehensive literature review has been published previously1
and can be found here
Although a number of detailed studies of snakebite have been conducted in Papua New Guinea2-5,
there has been no diminution of the burden that these encounters between
humans and reptiles produce1. Snakebite remains a common cause of
injury and death, especially for young, rural-dwelling people in southern
Papua New Guinea1. Analysis of mortality data at Port Moresby
General Hospital6 suggests that the treatment and management of
snakebite patients was not improved by previous clinical research conducted
more than a decade ago4-5. Looking further back to the earliest
studies of snakebite in PNG conducted by Dr C H Campbell in the 1960’s2,
it appears that the prognosis for patients has actually declined, rather
than improved1.
Campbell reported a case fatality rate of 6.8% after snakebite at Port Moresby General Hospital
(PMGH) during the years 1959 to 19652, and Price & Campbell gave
a mortality rate of 3.1% among 192 patients admitted to the hospital between
January 1967 and December 19717. In the 1980’s the case fatality
rate among children at PMGH was 7.7%3, but a study soon
afterwards found that while the overall case fatality rate between 1987 and
1992 was 4.4%, the rate among children was actually 10.0% compared to an
adult rate was 3.3%5.
Case fatality rates after snakebite at PMGH have continued to increase since the early 1990’s. A
study of snakebite deaths in the Intensive Care Unit (ICU) between 1992 and
2001 by McGain et al found that 87 of 722 patients died (12.0%), with
rates of 14.6% for children and 8.2% for adults6. Williams et
al studied ICU cases between 1998 and 2001 and found that 13.5% of
female snakebite patients died compared to only 7.7% of men8.
More recently a 12 month review of snakebite cases admitted to the ICU at
PMGH between September 2003 and August 2004 found an adult case fatality
rate of 14.5% and a paediatric case fatality rate of 25.9% (Unpublished
data: current study).
This apparent increase in mortality rates is an important focus of the research being
undertaken in the current study. Little is known of the determinants of
mortality outside the findings reported by McGain and colleagues as part of
their retrospective analysis of PMGH ICU admissions. By nature of the design
of their study, the data is limited to medical causes of death, and provides
no information on extraneous factors such as hospital systems failures. A
prospective study is being undertaken as part of this PhD research that
seeks to explore both the clinical and non-clinical contributors to
mortality and/or prolonged morbidity.
Current understanding of the syndromes of envenomation produced by particular
species has been well described by the student in a recent publication1.
The effects of bites by one species, the Papuan taipan Oxyuranus
scutellatus canni are well described9-12, although an
understanding of the mechanisms of some observed effects is not yet
available. Suspicion that venom from this species causes direct myocardial
toxicity has been suggested based on observed electrophysiological changes10,
but direct evidence of myocardial damage has not been presented. A
prospective study of troponin-I levels in patients with definite O.
scutellatus canni envenoming is being undertaken now in an attempt to
obtain quantitative evidence of myocardial damage after bites by this snake.
Descriptions of the effects of envenomation by other medically important species in PNG are
limited to a handful of small patient series13-16. Prospective
recruitment of patients with ELISA-proven envenoming by Papuan blacksnakes
Pseudechis papuanus, death adders Acanthophis spp., and
small-eyed snakes Micropechis ikaheka to a study of haemostatic and
biochemical changes will significantly improve our understanding of the
individual syndromes of envenoming produced by these taxa.



Conceptual framework and description of project components
The research being undertaken seeks to resolve a number of the outstanding issues relating to
not just the treatment of snakebite patients, but also addresses the broader
topics of surveillance and reporting, resource allocation, public health
education, workforce training and fundamental scientific research.
Broadly speaking the overall project is a conglomeration of several smaller inter-related
research activities being conducted in various locations in Papua New
Guinea. These individual projects can be grouped as:
-
National epidemiological analysis;
-
Development of tools for surveillance & mapping;
-
Snakebite studies;
-
Phylogenetic and biogeographical studies;
-
Health system capacity building.
This approach therefore aims to:
-
Establish models for the future reporting and monitoring of snakebite-related data;
-
Develop analytical tools with which to query the information;
-
Further define envenomation syndromes;
-
Seeks solutions to clinical care questions;
-
Define species limits and identify new forms of venomous taxa;
-
Develop local capacity at all levels and transfer the results of the research.
The research is taking place in Papua New Guinea, at various locations in close consultation
with the PNG National Department of Health who are David Williams' sponsors,
and with both local administrators and clinicians. The individual projects
that comprise the research are listed below. Projects involving human or
animal research have been approved by either the PNG Medical Research
Advisory Committee, or the University of Papua New Guinea Medical Ethics
Committee.



Epidemiology of snakebite in Papua New Guinea – a national analysis
Development of snakebite surveillance and mapping technology
Collaboration with University of Melbourne, Department of Geomatics personnel:
-
Epidemiological, zoogeographical, topographic and climatic data is being incorporated
into a snakebite mapping application developed in collaboration with
UniMelb Dept of Geomatics;
-
A mapping interface has been developed that can operate either from a PDA device
or personal computer;
-
Application will be used to analyse the relationship between variables (eg.: geology,
rainfall, aspect, vegetation, etc.) and snakebite incidence;
-
Objective is to identify potential higher risk areas in specific regions of PNG and gain
understanding of the determinants.
Morbidity and mortality after snakebite at Port Moresby General Hospital
Prospective clinical study in collaboration with local medical officers and visiting emergency
physicians:
-
Investigates the causes of prolonged morbidity and/or high mortality after snakebite;
-
Consists of retrospective chart analysis and prospective patient recruitment to a 12
month study of outcomes in the high dependency and intensive care units
at PMGH;
-
Explores both the medical causes and the contributing systems issues;
-
Objective: improved management by identifying and reducing system failures.


Cost-benefit trial of snake venom detection kits in Papua New Guinea
Prospective study of benefits associated with the use of CSL SVDKs:
-
Based on protocol whereby all patients with early clinical signs of envenoming
are subjected to a SVDK test using either a bite site swab or urine
sample;
-
Antivenom timing and choice are based on the rest of the SVDK test;
-
Objective is to trial a protocol for SVDK use and quantify the potential clinical and
financial benefits;
-
Effect measures will be used to determine whether the introduction of routine SVDK use
in Papua New Guinea is economically and medically justified.
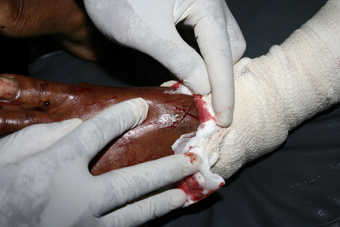
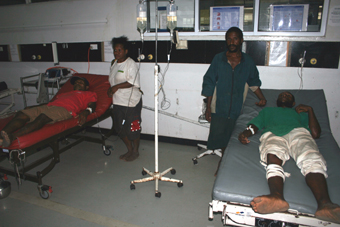
Changes in haemostasis, serum isoenzymes and troponin levels after snakebite in Papua
New Guinea
Prospective clinical study of effects of the venoms of particular species on coagulation enzymes,
liver function, skeletal and cardiac muscle:
-
Patients with a positive SVDK test are being recruited to the study prospectively;
-
Aim is to identify specific syndromes associated with bites involving particular
venom immunotypes and to expand current knowledge of the clinical
effects of different snake venoms;
-
Hopeful of recruiting subjects envenomed by Acanthophis spp., Pseudechis
papuanus, and Micropechis ikaheka as little is known
regarding envenomation by these species in Papua New Guinea;
-
Results will improve understanding of envenomation syndromes and be used to improve
the quality of clinical management and care provided to patients.


Efficacy of snakebite first aid training in rural Papua New Guinea
Study to trial a training system for teaching rural people how to correctly apply PIB:
-
System uses positive feedback to reinforce the need to apply bandages at optimal
tensions and regular re-testing to evaluate skill retention;
-
Aim is to quantify the efficacy of application by trainees over time as a test of
skill retention and hence training program efficacy;
-
Project is based in two rural communities on Karkar Island off the coast of Madang;
-
Objective is to determine the likelihood for success of a large scale PIB-education and
training project throughout rural Papua New Guinea.
Validation of 20 minute whole blood clotting test
Investigate the reliability of the 20WBCT under normal conditions of use:
-
Aim is to determine the PPV, NPV, sensitivity and specificity of the test in
untainted blood samples, and in samples containing venom from each
medically important species;
-
The study design trials the reliability in different types of glassware and seeks to
determine false-positive rates in healthy volunteers;
-
Also tests for Inter-rater variability among clinicians who would normally be
responsible for interpreting the result of a 20WBCT in clinical
practice.


Clinical study of an anticholinesterase use protocol for death adder (Acanthophis spp.)
envenoming in PNG
Prospective study of the efficacy of a trial protocol for the use of neostigmine and atropine as
primary therapy for death adder envenomation in PNG:
-
Project seeks to examine the efficacy, safety and duration of effect using quantitative
measurements of neurotransmission recovery;
-
Study to be based at Gaubin hospital on Karkar Island where death adders are the
predominant biting species;
-
Other hospitals in Madang province may also be involved subject to personnel being
available to participate in the project;
-
Study will compare the use of anticholinesterases against the efficacy and safety
of CSL death adder antivenom.


-
In vivoefficacy of current antivenoms unknown although CSL polyvalent believed
effective based on in vitro studies;
-
Prospective study at Gaubin hospital on Karkar Island aims to describe the syndrome
of envenoming and assess the clinical efficacy of CSL polyvalent
antivenom.
Antivenom binding studies: affinity for PNG small-eyed snake (Micropechis ikaheka)
venom
-
Investigation of venom neutralisation after antivenom administration;
-
Study will use quantitative ELISA techniques to measure venom and antivenom levels in
serial samples taken from envenomed patients;
-
Coupled with laboratory-based 2D PAGE and western blotting studies to determine
binding of individual venom components to antivenom.


Phylogenetics and biogeography of Australo-papuan venomous snakes
-
Collaborative research project with Dr Wolfgang Wüster (AVRU Honorary Fellow);
-
Investigation of relationships between disjunct populations within the same taxa, and of
the inter-relationships between members of same genera;
-
The aim is to determine species limits and identify new taxa that may produce
different clinical syndromes as a result of venom variation;
-
Variations in venoms may enable identification of new toxin candidates;
-
cDNA libraries will be constructed using venom glands from disjunct populations.
Public health capacity building
Public health management project involving the development of local capacity and
establishing new infrastructure and resources, with components that include:
Systems and infrastructure development:
-
National Antivenom Unit at UPNG to coordinate the acquisition and distribution of
antivenoms and to conduct epidemiological surveillance;
-
Collaborative development of basic research capacity & facilities at the University of
Papua New Guinea’s School of Medicine and Health Sciences.
Relevance and importance
Papua New Guinea is Australia’s nearest neighbour, and shares with us, many of the same genera
and species of venomous animals. This means that envenomation problems in
PNG have relevance to the treatment of envenomation in rural and remote
regions of Australia. Since the incidence of envenomation in PNG is
considerably higher than it is in Australia, the opportunities for
undertaking meaningful research with sample sizes sufficient to establish
statistical relevance are greatly enhanced. The practical nature of the
research also has direct relevance to both the treatment of envenomation in
PNG and in Australia.
Within a broader context the approach being undertaken also has relevance to the issue of
envenomation throughout many other parts of the tropical world, and in
particular, within developing countries which often experience the greatest
challenges in dealing with snakebite prevention, treatment and surveillance.
The aim of the research is to combine several different areas of research in
order to produce a functionally sustainable improvement in the overall
management of snakebite as a health problem in Papua New Guinea. The ‘tools’
that are being developed and trialled in PNG are transferable to other
settings, and a key objective of the research is to develop a set of
research techniques and tools that can be used in other parts of the world
to produce similarly sustainable results.
As a global problem, snakebite may affect the lives of up to 4 million people a year throughout
the world, yet there is currently no global push for coordinated research to
reduce the burden of what is essentially a preventable and treatable
illness. The work being undertaken here is an important step towards
positioning AVRU to be a driving force behind just such a global initiative.
Bibliography
-
Williams DJ, Jensen SD, Nimorakiotakis B, Winkel KD (Eds). Venomous Bites and
Stings in Papua New Guinea: A Treatment Guide for Health Workers and
Doctors. Australian Venom Research Unit, Melbourne, September 2005,
416 pp. ISBN 0-975937-0-5.
-
Campbell CH. A clinical study of venomous snakebite in Papua. MD thesis,
1969, University of Sydney.
-
Brian MJ, Vince JD. Treatment and outcome of venomous snake bite in children,
Port Moresby General Hospital, Papua New Guinea. Trans R Soc Trop
Med Hyg 1987; 81: 850-2.
-
Currie BJ, Sutherland SK, Hudson BJ, Smith AM. An epidemiological study of
snakebite envenomation in Papua New Guinea. Med J Aust 1991;
154: 266-268.
-
Lalloo DG, Trevett AJ, Saweri A, et al. The epidemiology of snakebite in
Central Province and National Capital District, Papua New Guinea.
Trans Roy Soc Trop Med Hyg 1995; 89:178-182.
-
McGain F, Limbo A, Williams DJ, et al. Severe Snakebite at Port
Moresby General Hospital, Papua New Guinea 1992-2001. Med J Aust
2004; 181: 687-691.
-
Price M, Campbell CH (1979) Snake bite admissions PMGH 1967-1971. PNG Med
J; 19: 155
-
Williams DJ, Kevau IH, Hiawalyer GW, et al Analysis of Intensive Care
Unit admissions for treatment of serious snakebite at Port Moresby
General Hospital. Proceedings of the 11th Annual Scientific
Meeting of the Australasian College of Tropical Medicine and the 6th
Asia-Pacific Congress of the International Society of Toxinologists
.Cairns, Australia (July 8-12, 2002).
-
Lalloo DG, Hutton R, Black J, et al. (1993) Mechanisms of coagulopathy
following envenoming by the Papua New Guinean Taipan. Toxicon.
31(8):937
-
Lalloo DG, Trevett AJ, Nwokolo N, et al. (1997) Electrocardiographic
abnormalities in patients bitten by taipans (Oxyuranus
scutellatus canni) and other elapid snakes in Papua New Guinea
Trans Roy Soc Trop Med Hyg. 91(1):53-6.
-
Lalloo DG, Trevett AJ, Kornihona A, et al. (1995a) Snake bites by the
Papuan taipan (Oxyuranus scutellatus canni): Paralysis,
hemostatic and electrocardiographic abnormalities, and effects of
antivenom. Am J Trop Med & Hyg. 52(6): 525-31.
-
Trevett AJ, Lalloo DG, Nwokolo NC, et al. (1995b) The efficacy of
antivenom in the treatment of bites by the Papuan taipan (Oxyuranus
scutellatus canni) Trans Roy Soc Trop Med Hyg. 89:322-25.
-
Campbell CH. (1966) The death adder (Acanthophis antarcticus): the
effect of the bite and its treatment. Med J Aust. 2:922-925
-
Lalloo DG, Trevett AJ, Black J, et al. (1996) Neurotoxicity
anticoagulant activity and evidence of rhabdomyolysis in patients
bitten by death adders (Acanthophis sp.) in southern Papua
New Guinea. Q J Med. 89:25-35.
-
Lalloo D, Trevett A, Black J, et al. (1994) Neurotoxicity and
haemostatic disturbances in patient's envenomed by the Papuan black
snake (Pseudechis papuanus). Toxicon. 12(8):927-936.
-
Warrell DA, Hudson BJ, Lalloo DG, et al. (1996) The emerging syndrome
of envenoming by the New Guinea small-eyed snake Micropechis
ikaheka. Q J Med. 89:523-30.





















